Home » Articles posted by Wendy Jones (Page 8)
Author Archives: Wendy Jones
Clinically extremely vulnerable, COVID 19 infection and breastfeeding
Because I am immunocompromised myself, I am all too well aware of the information on protection from COVID 19 including the recommendations launched in December 2021 by the government on sotrovimab (Xevudy) and molnupiravir (Lagevrio) . This may affect some breastfeeding mothers e.g. those with IBD or on biologicals for other reasons . There are no simple answers but this is the information I have been able to find in one place. The factsheet was updated in April 2022 following the licence change by the FDA of sotrovimab, and added data on Evusheld and remdesivir .
In January 2023 the WHO changed guidelines on the preferred therapies and compatability with the drug which they recommend and breastfeeding. This is the information which I have been able to access
https://breastfeeding-and-medication.co.uk/wp-content/uploads/2023/01/COVID-19-and-CEV-jan-2023.pdf
Update WHO Guidelines January 2023 https://www.who.int/publications/i/item/WHO-2019-nCoV-therapeutics-2023.1
NICE TA 878 March 2023 Casirivimab plus imdevimab, nirmatrelvir plus ritonavir, sotrovimab and tocilizumab for treating COVID-19 https://www.nice.org.uk/guidance/ta878
In October 2023 the Specialist Pharmacy Service (SPS) reported that breastfeeding can continue as normal during COVID-19 infection, even if dexamethasone, Paxlovid, sotrovimab or tocilzumab are required. COVID-19 vaccines can also be given. https://www.sps.nhs.uk/articles/managing-covid-19-and-breastfeeding
nirmatrelvir-ritonavir (Paxlovid)
- The GDG concluded that nirmatrelvir-ritonavir represents a superior choice because it may have greater efficacy in preventing hospitalization than the alternatives; has fewer concerns with respect to harms than does molnupiravir; and is easier to administer than intravenous remdesivir and the antibodies.
- Clinicians should review all medications and not consider nirmatrelvir-ritonavir in patients with possible dangerous drug interactions (note: many drugs interact with nirmatrelvir-ritonavir).
- Fully informed shared decision-making should determine whether nirmatrelvir-ritonavir should be used in pregnant or breast-feeding women, given possible benefit and residual uncertainty regarding potential undesirable effects.
- Nirmatrelvir-ritonavir should be administered as soon as possible after onset of symptoms, ideally within 5 days.
- Data on breastfeeding from expert sources is in the link but two case reports in which nirmatrelvir/ritonavir was given to breastfeeding women did not report any adverse effects in their infants.
casirivimab-imdevimab strongly recommended against use
sotrovimab strong recommendation against use because neutralization of currently circulating variants of SARS-CoV-2 and their subvariants with sotrovimab is diminished.

Bi polar disorder and breastfeeding
This is one section of the new book on chronic medical conditions and breastfeeding. It is available on Amazon as a kindle or paperback book .
I have updated the information in view of the information shared by Specialist Pharmacy Service October 2023 https://www.sps.nhs.uk/articles/treating-bipolar-disorder-during-breastfeeding/
“I was only diagnosed with bipolar during my first pregnancy so breastfeeding was very much uncertain and a lot of healthcare professionals maybe weren’t so keen but I fed my eldest until he was 13 months when he self-weaned as I was pregnant with my second. I would love to be able to help anyone I can, I am very passionate about breastfeeding and honestly think it has been a real stabilising factor in my mental health!”
“Medication to control the symptoms of bipolar disorder is complicated. If we add in the emotional turmoil that occurs post-delivery and lack of sleep, there may need to be regular review. Mothers have been known to come off their medication in order to breastfeed with dire consequences. We need to provide them with evidence-based information to understand the risks and benefits of the treatment regime. (A professional viewpoint)”
Description
Bipolar disorder is a mental health condition that affects moods. The latter can swing from one extreme of lethargy and depression to a feeling of being high and overactive hence the original name of manic depression.
During bouts of depression it is not uncommon to feel suicidal or worthless and it is important to recognise this and seek a place of safety or a person you trust as quickly as possible. During a manic phase there may be feelings of having lots of energy, ambitious plans and idea. It is not uncommon to spend large amounts of money on expensive, unwanted goods and some people ask their banks to block spending above a certain level to avoid debt. It is also common to not feel like eating or sleeping, to talk quickly and become easily annoyed. For some this phase is a positive experience and a time of creativity so may reject medication. It may also become a psychotic phase where things which do not exist may be seen and heard (voices controlling actions). It is a complex condition which may need adjustments. Around one in every 100 people will be diagnosed with it at some point in their life. It frequently develops between 15 and 19 years of age but rarely after 40. The incidence is the same in men and women. The pattern of mood swings in bipolar disorder varies widely. Some people only have a couple of episodes in their lifetime and are stable in between, while others have many episodes.
Diagnosis is made only after one episode of mania as well as the depression. In this state the mother may have an elated mood or alternatively she may feel irritable and angry. She may experience racing thoughts rapidly changing from one area to another. It may be impossible for her to be still, but the activity may be unproductive. It is reported to affect a higher proportion of intelligent people with gifted creativity.
Treatment
Anti-depressants: See Section on Depression
mood stabilisers :
carbamazepine: reaches relatively high levels in breastmilk but does not appear to affect growth or development. Sedation, poor feeding, withdrawal reactions and 3 cases of hepatic dysfunction have been reported but maybe due to placental transfer
valproate: If valproate is taken during pregnancy, around 1 in 10 babies are born with birth defects and up to 4 in 10 babies will have developmental problems. It is no longer recommended in pregnancy and has in consequence fallen out of use in breastfeeding. If this is the best suited drug it is compatible with breastfeeding, but the mother should take adequate contraceptive precautions. Valproic acid levels in breastmilk are low and infant serum levels range from undetectable to low. theoretically it is recommended that the baby should be monitored for jaundice and liver damage if clinical symptoms present (Hale online). Valproate can be used during breastfeeding in the management of bipolar disorder (SPS) but with adequate contraceptive methods.
Resources for healthcare professionals and patients https://www.rpharms.com/resources/pharmacy-guides/valproate-and-the-pregnancy-prevention-programme
- Patient card – to be given by pharmacists to all female patients who are dispensed valproate medicines to inform them of the risks
- Patient guide – to be provided to girls (of any age) and women of childbearing potential (or their parent/caregiver/responsible person) taking any medicine containing valproate
- Guide for healthcare professionals – for all prescribers, pharmacists, and other healthcare providers involved in the care of women and girls of childbearing potential using valproate medicines
- Annual risk acknowledgement form – (revised November 2019) for the specialist and patient (or their parent/caregiver/responsible person) to sign at initiation and at treatment reviews at least every year – the patient should receive a copy of the form; one copy should be filed in the specialist notes, and one copy sent to the patient’s GP.
lamotrigine: Relatively high plasma levels have been reported in breastfed babies. Neonates are particularly susceptible due to their inability to metabolise the drug if the dosage is not reduced to the pre-pregnancy dosage in the immediate post-partum period. Relative infant dose is quoted as 9.2-18.3%. Page-Sharp (2006) studied six breastfeeding women taking a mean dose of 400 mg per day of lamotrigine. Five of the babies were exclusively breastfed and the remaining one fed with half breastmilk and half artificial milk feeds. No adverse events were noted in any of the infants. In general infants should be monitored for sedation, feeding difficulties, adequate weight gain and developmental milestones.
lithium: Has historically been described as not compatible with breastfeeding unless baby can be monitored with monthly blood tests. However October 2023 SPS reported that “Lithium can also be used for the management of bipolar disorder, but must be with extreme caution, under specialist supervision, and with strict infant monitoring conditions.” Lactmed (https://www.ncbi.nlm.nih.gov/books/NBK501153) states that “Lithium excretion into breastmilk and concentrations in infant serum are highly variable, and that numerous reports exist of infants who were breastfed during maternal lithium therapy without any signs of toxicity or developmental problems. Most were breastfed from birth and some continued to nurse for up to 1 year of maternal lithium therapy. The baby would need regular blood tests to monitor, just as the mother does . The infant should be monitored for Neurobehavioral development, drowsiness, irritability, dry mouth or excessive salivation, thyroid function, vomiting, constipation, hydration, renal function, urination, tremor. The decisions should be taken with full information
.
Atypical antipsychotics:
risperidone (Risperidal™): Limited information indicates that maternal risperidone doses of up to 6 mg daily produce low levels in milk. Observe baby for drowsiness but no adverse events reported to date.
olanzapine (Zyprexa™): Maternal doses of olanzapine up to 20 mg daily produce low levels in milk and undetectable levels in the serum of breastfed infants. Monitor the baby for drowsiness and effective feeding.
quetiapine (Seroquel™): Maternal quetiapine doses of up to 400 mg daily produce low levels in milk. Monitor the baby for drowsiness and effective feeding.
ariprazole (Ablify ™): Limited information indicates that maternal doses of aripiprazole up to 15 mg daily produce low levels in milk. However, it inhibits prolactin levels and despite expert advice it may not be possible to achieve a full milk supply ((Mendhekar 2006, Nordeng 2014).
Choice of medication must be guided by clinical need, but it is usually, depending on the dose, possible to continue to breastfeed. If it is not possible, the mother and her family should be consulted in making an informed choice.
References
- Hale TW Medications and Mothers Milk Online access
- Mendhekar DN, Sunder KR, Andrade C. Aripiprazole use in pregnant schizoaffective woman. Bipolar Disord 2006; 8:229-300
- Nordeng H, Gjerdalen G. BRede WR, Michelsen LS, Spigset O. Transfer of aripiprazole to breast milk: a case report. J Clin Psychopharamcology 2014;34(2):272-75.
- Page-Sharp M, Kristensen JH, Hackett LP, Beran RG, Rampono J, Hale TW, Kohan R, Ilett KF, Transfer of lamotrigine into breastmilk, Ann Pharmacother, 2006;40:1470–1, Letter.
- SPS Treating bipolar disorder during breastfeeding https://www.sps.nhs.uk/articles/treating-bipolar-disorder-during-breastfeeding
Further information:
BiPolar UK www.bipolaruk.org

Biotin and Products to support hair growth/ thickness
It is normal during lactation to notice that your hair becomes thinner or may even appear to drop out in significant levels. In pregnancy we grow more hair and the apparent loss is usually just a return to normal.
It may however, be a sign of thyroid deficiency so always worth checking with your doctor and requesting a blood test to check levels, just in case. Biotin can interfere with thyroid tests so better avoided until this has been ruled out as a cause of hair thinning (October 2023 https://www.nice.org.uk/guidance/ng145/chapter/Update-information).
Most of the commercially available products which claim to thicken, strengthen, promote growth of hair contain biotin in addition to the normal vitamins and minerals.
Symptoms of biotin deficiency include thinning hair, skin rash, and depression. The recommended daily dose of biotin for a lactating woman is 35 µg/day. Levels of biotin in human milk range from 5 to 9 µg/L, indicating that there is active transport of biotin into milk. No adverse effects have been found. (Hale Medications and Mother’s Milk)
Biotin (vitamin B7) is needed in very small amounts to help the body break down fat. The bacteria that live naturally in the bowel synthesise biotin, so it’s unclear whether supplements are necessary if a varied and balanced diet is eaten.. Biotin is also found in a wide range of foods, but only at very low levels. There’s not enough evidence to know what the effects might be of taking high daily doses of biotin supplements. Taking 0.9mg or less a day of biotin in supplements is unlikely to cause any harm. ( NHS Vitamin B https://www.nhs.uk/conditions/vitamins-and-minerals/vitamin-b/)
Vitamin and Mineral content compatible with breastfeeding https://breastfeeding-and-medication.co.uk/fact-sheet/breastfeeding-and-multivitamin-and-mineral-supplements

Miscarriage and Breastfeeding
I’ve realised that the information I wrote long ago now, on loss of a pregnancy and breastfeeding is not very detailed so I have written a more detailed factsheet. My heart goes out to everyone who has to go through the loss of a baby through miscarriage. We don’t talk about it openly often enough considering how common it is .
If the baby is lost whilst you are still breastfeeding an older child your milk supply may suddenly increase. If your child isn’t feeding as frequently you may risk mastitis so please be aware if you suffer engorgement and your nursling doesn’t remove the full supply.
If the miscarriage is late in pregnancy then milk production may still begin and this may come as a shock see https://breastfeeding-and-medication.co.uk/fact-sheet/stillbirth-and-milk-supply
Sending hopeful rainbows for the future

miscarriage and breastfeeding factsheet
Sometimes longed-for pregnancies end in miscarriage. The signs of miscarriage may be vaginal bleeding and cramps in the lower abdomen. You may need to take painkillers as you would for period pains. Sometimes not all the ‘products of conception’ may be expelled. You may be monitored by the early pregnancy unit who will scan your uterus and advise accordingly. You may be treated elsewhere in the hospital.
However, you may find yourself in the heart-breaking situation of attending for a scan to be told that your baby has no heartbeat and died some time ago. You may not have had any symptoms that a problem has occurred but with hindsight may recognise that symptoms of morning sickness had eased. This is called a missed or silent miscarriage.
You may be given drugs to bring on the miscarriage (medical management) or you may be offered an operation to make sure the womb is clear (surgical management), You may prefer to wait for nature to take its course and your body to expel the baby in its own time – this happens in around 50% of cases. The decision is yours after a fully informed discussion with those caring for you and your family.
Medical management
You can continue to feed as normal after misoprostol and after mifepristone https://www.sps.nhs.uk/articles/medically-terminating-a-pregnancy-during-breastfeeding/
Some units use mifepristone tablets to break down the lining of the uterus and you can feed as normal after taking that drug. Normally you return for the second tablets after 48 hours, but this alone may bring on the miscarriage in some women.
You may alternatively be given a single dose of misoprostol vaginally. Or you may be offered a two-stage medication procedure: a mifepristone 200mg tablet orally followed 24–48 hours later by misoprostol 800 micrograms. This is usually given as a pessary but can be a tablet under the tongue (sub lingually). You may also be given painkillers, anti-sickness tablets and antibiotics. You can continue to breastfeed an older baby 4 hours after the misoprostol to avoid risks of diarrhoea in your nursling although Hale suggests that this may be unnecessary. The misoprostol helps the neck of the womb (cervix) to open and lets the remaining pregnancy come away.
Pain and bleeding usually occur within one to two hours of using misoprostol. Often bleeding is heavy with clots. It is not unusual to soak four to six pads in the first hour. You may see the pregnancy sac when it passes, but you will probably not see a recognisable baby if it is still very early in the pregnancy. Most women experience strong cramps and abdominal pains. These pains are usually strongest while the bleeding is heavy and should ease off quite quickly once the pregnancy remains have passed. You can use pain relief medication such as ibuprofen, paracetamol and dihydrocodeine.
If bleeding does not start within 24 hours you need to contact the unit looking after you.
Surgical management
As soon as you are awake and alert following surgery you can continue to breastfeed your nursling as normal
You may be offered, or ask for, surgical removal of the miscarriage although this is much less common due to the effectiveness of the medication and that you can take that at home.. Surgery will involve a general or local anaesthetic and you can feed as normal as soon as you are awake and alert. This procedure can be called a D and C or an ERPC when performed under GA but an MVA when under a local anaesthetic The pregnancy is removed through the cervix. You may be given tablets to swallow or vaginal pessaries before the operation to soften your cervix. These do not affect breastfeeding. Surgery will usually take place within a few days of your miscarriage, but you may be advised to have surgery immediately if you are bleeding heavily and continuously or there
are signs of infection. It may also be offered if medical treatment to remove the pregnancy has been unsuccessful.
Following the miscarriage
It is important to give yourself time to grieve – this was the loss of a dream as well as a baby. It is common to feel guilty as well as sad. Many families don’t share the news of a pregnancy until after the 12-week scan ‘just in case’, but if something happens you need friends to care for you, so consider letting them know what’s happened.
The reasons for miscarriage are many and varied. in women under 30, 1 in 10 pregnancies will end in miscarriage. It is common but something we rarely talk about openly. Just because it has happened once does not increase the chances of it happening again but quite naturally you will worry. Most people are advised to wait a full cycle before trying to conceive again to give mind and body time to heal. It also makes dating of the next pregnancy easier if conception does occur rapidly.
See https://www.nhs.uk/conditions/miscarriage/causes/ for more information.
Prevention of recurrent miscarriage
Some women experience recurrent miscarriages and need to take medication in order to protect the foetus. This may include the use of 75 -150mg aspirin, progesterone pessaries and low molecular weight heparin injections. All of these are compatible with normal breastfeeding. About 1 in 100 women experience recurrent miscarriages (3 or more in a row) and many of these women go on to have a successful pregnancy
What happens to the remains of the pregnancy?
Many people pass the pregnancy sac whilst on the toilet. Some people choose to just flush the toilet or do so automatically. Some want to look more closely first. Others choose to bury it in the garden maybe near a shrub or flowers. All these reactions are normal and individual. There is no right or wrong. Do what feels the right thing for you. You will not ever forget this day, this baby or this little one’s due date. Hopefully in the future you will have your Rainbow baby (a baby born subsequent to a miscarriage, stillbirth, or the death of an infant from natural causes).
References and Resources
- Breastfeeding and Medication. Jones W Routledge 2017
- BPAS Medical management of miscarriage. Accessible from: https://www.bpas.org/more-services-information/miscarriage-care/medical-management/
- Guys and St Thomas Medical Management of Miscarriage. Accessible from: https://www.guysandstthomas.nhs.uk/resources/patient-information/gynaecology/medical-management-of-miscarriage.pdf
- Hale TW Medications and Mothers milk (online access)
- LactMed https://www.ncbi.nlm.nih.gov/books/NBK501922/
- NHS Miscarriage: Accessible from: https://www.nhs.uk/conditions/miscarriage/
- NICE NG 126 Ectopic pregnancy and miscarriage: diagnosis and initial management. Accessible from https://www.nice.org.uk/guidance/ng126
- Royal College of Obstetrics and Gynaecology Early Miscarriage patient information leaflet. Accessible from: https://www.rcog.org.uk/globalassets/documents/patients/patient-information-leaflets/pregnancy/pi-early-miscarriage.pdf
- The Miscarriage Association https://www.miscarriageassociation.org.uk/
- The Miscarriage Association Management of Miscarriage. Accessible from: https://www.miscarriageassociation.org.uk/wp-content/uploads/2016/10/Management-of-Miscarriage-April-2019.pdf
- “Why Mothers Medication Matters” Jones W Pinter and Martin 2017
This information is dedicated to the two grandchildren I never got to meet


Ear drops and breastfeeding
Continuing to work down the list of frequently asked questions and adding information from Breastfeeding and Medication 2018
If you are a professional or a volunteer frequently encountering questions from mothers or other members of the family maybe you would like to treat yourself to a copy!
The ear drops I am asked about most frequently asked about are OTOMIZE and LOCORTEN VIOFORM but this fact sheet contains many others. Hope it puts everyone’s mind at rest. I remember a consultant many years ago telling a mother she couldn’t breastfeed for 2 weeks after using anti inflammatory ear drops. Unless she was going to drip excess out of the ear canal onto her nipples I could see no logic for this. I hope things have moved on but the patient information leaflet still causes concern.
pdf of factsheet available ear drops and breastfeeding
Absorption of ear drops is unlikely to reach clinical significance in breastmilk as there is virtually no means of absorption into the systemic system from the external ear canal.
Ear drops generally include corticosteroids to reduce inflammation, antibiotics to reduce otitis external, antifungals, local anaesthetics for pain and ingredients to soften and remove earwax. Treatment of otitis media with ear drops is generally ineffective and is better treated by simple analgesia and, if necessary, antibiotics. Almond oil, olive oil and sodium bicarbonate solution are all used to soften ear wax.
Examples of ear drops and their ingredients:
Betnesol N® Betamethasone And Neomycin)
Betnesol® (Betamethasone),
Cerumol® (Chlorbutanol),
Gentisone HC® (Gentamicin And Hydrocortisone)
Gentisone® (Gentamicin)
Locorten-Vioform® (Flumetasone And Clioquinol)
Neo-Cortef® (Hydrocortisone And Neomycin)
Otex® (Urea Hydrogen Peroxide)
Otomize® (Dexamethasone, Neomycin And Acetic Acid)
Otosprorin® (Polymyxin B Neomycin Hydrocortisone)
Predsol N® (Prednisolone And Neomycin)
Predsol® (Prednisolone)
Sofradex® (Dexamethasone Framycetin Gramicidin)

Naproxen and Breastfeeding
Naproxen is frequently used as an anti inflammatory and to add pain relief for instance after surgery. However, there seems to be concern about prescribing it for the breastfeeding mother. I hope this information helps.
pdf of information Naproxen and Breastfeeding factsheet
If it was useful maybe you need to buy the book?
Naproxen is an anti-inflammatory drug used more frequently since concerns were raised about long term cardiovascular risk of diclofenac. It is generally seen as more effective than ibuprofen. Concerns have been raised that its longer half life produces more of a risk to a breastfeeding baby. It is only taken twice a day at 12 hourly intervals.
Naproxen is more than 99% bound to plasma proteins. Davies and Anderson (1997) reported that although naproxen is excreted into breastmilk, the amount of drug transferred comprises only a small fraction of the maternal exposure. Relative infant dose quoted as 3.3% (Hale 2023 online access) lower than 10% regarded as compatible with breastfeeding.
In Jamali and Stevens’ study (1983) only 0.26% of the mother’s dose was recovered from the infant and adverse effect reports are low.
The BNF considers that the amount of naproxen distributed into breastmilk is too small to be harmful to a breastfed infant; however, some manufacturers recommend that breastfeeding should be avoided during naproxen therapy, due to licensing considerations rather than potential risk.
References see Breastfeeding and Medication Text

Quitting Smoking During Pregnancy And Beyond
Introduction
Before I start talking about quitting smoking, I want to acknowledge that it isnt easy. Nicotine is very addictive, and everyone smokes for their own reasons. Everyone has a habit they would like to break: mine is enjoying too much chocolate. To stop doing anything which you enjoy takes guts and a lot of will power. Maybe your baby is your reason to quit but it also needs to be because YOU want to not just because you have been TOLD to. I hope this information helps you but always happy to help if you want to email me wendy@breastfeeding-and-medication.co.uk
Smoking in Pregnancy
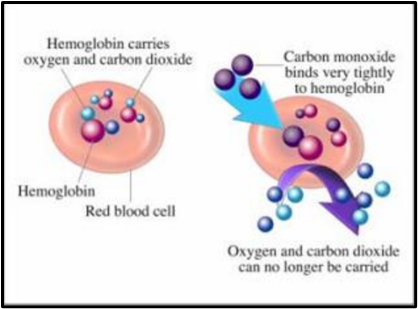
We know that smoking during pregnancy is associated with risk factors to the baby including low birth weight at delivery, increased risk of miscarriage or stillbirth because carbon monoxide in tobacco smoke reduces the amount of oxygen getting to the placenta and the baby . There are also future risks of respiratory problems including ear, nose and throat. However as at 2020/21 9.5% of women were smoking at the time of delivery which was the lowest on record.
In a 2010 study by the Office of National Statistics (ONS) 14% of women were smoking before pregnancy but gave up, 12% continued to smoke throughout pregnancy although 9% cut down. The study showed that 1% gave up but went back to smoking during the pregnancy.
A report published by the Royal College of Physicians in 2010 estimated that in the UK, smoking during pregnancy causes up to 5,000 miscarriages, 300 deaths around the time of birth and approximately 2,200 premature births each year.

(taken from https://ash.org.uk/resources/view/smoking-pregnancy-and-fertility)
Why do mothers smoke during pregnancy?

Why, might we ask, knowing that smoking during pregnancy is harmful to the baby do so few expectant mothers not quit? The answer is very simple: nicotine is extremely addictive and it is hard to break the habit of smoking. Just as overwight people know that they need to lose weight, try to diet but often return to their original weight or more.
Smoking is often linked to deprivation and women may smoke because they cannot afford to eat. If you live with someone else who smokes, you are six times more likely to smoke throughout pregnancy. Additionally, those who live with a smoker and manage to quit are more likely to relapse once the baby is born. If all your friends smoke, especially if you are younger, it is much harder to quit so peer pressure has much to answer to.
How can you stop smoking?
Over half (53%) of the women in a large 2010 study had been given information on how to stop smoking, and a third had received information on how to cut down smoking (32%) and how their partner could stop smoking (33%) but still had not quit. Maybe you have been given the information and now want to quit but have felt “nagged” into doing so when you aren’t ready?
Midwives, pharmacists, GPs as well as smoking cessation clinics can provide nicotine replacement products. These are free on the NHS whilst you are pregnant.
In April 2023 Health Minister Neil O’Brien announced that following the success of local schemes, pregnant women will be offered financial incentives to help them stop smoking. This will involve offering vouchers, alongside behavioural support, to all pregnant women who smoke by the end of 2024.
Nicotine replacement therapy

You can use nicotine replacement therapy (NRT) during pregnancy if it will help you stop smoking and you’re unable to stop without it. It’s not recommended that you take stop smoking tablets such as Champix or Zyban during pregnancy.
Smoking cessation interventions have been shown to reduce the number of new-borns with low birth weight and preterm births. In one study, compared to ongoing heavy smoking, quitting was associated with a 299g increase in birth weight. The less a premature baby weighs at birth the more interventions it is likely to need and the longer it will stay in NICU (neonatal intensive care unit).
NRT contains only nicotine and none of the hundreds of other damaging chemicals found in cigarette smoke. Tobacco smoke contains over 7,000 chemical compounds. NRT is a better option than continuing to smoke. It helps you by giving you the nicotine you would have had from a cigarette whilst you break the habit of reaching for a cigarette ( see below for how to break the habit of smoking).
NRT is available as:
- Patches (The 16-hour NRT patches are preferred to the 24-hour period ones)
- gum
- inhalator
- nasal spray
- mouth spray
- oral strips
- lozenges
- micro tabs
Sometimes a combination of a sustained release patch together with a rapid delivery method works well. As a pharmacist smoking cessation advisor, I often found that the people I was working with found it easier if they had something to hold in their mouths or their hands, so benefitted from an inhalator even if it didn’t contain a product.
Vaping and pregnancy

The vapour from an e-cigarette does contain some of the potentially harmful chemicals found in cigarette smoke, but at much lower levels. If using an e-cigarette helps you to stop smoking, it is much safer for you and your baby than continuing to smoke.
E-cigarettes may be more effective than nicotine patches for pregnant women trying to quit smoking, research found. One major study did not raise any new safety concerns with e-cigarettes (vaping) in pregnancy.
Smoking and breastfeeding
- Nicotine is found in breastmilk of mothers who smoke together with Cotinine, Cadmium, Mercury, Lead and other heavy metals, and a lower amount of proteins, Vitamin A, C and E and other antioxidants.
- The flavour of breastmilk collected 30-60 minutes after smoking was identified as tasting more like cigarettes than samples taken at any other time.
- The levels of cotinine (the chemical into which nicotine is changed in the body) in the urine of breastfed babies whose mothers smoked were ten times higher than those of formula fed babies of smoking mothers. It appears that this is due to passage through breastmilk and not through exposure to smoke in a room.
- Babies of mothers who smoke appear to be more likely to suffer from colic.
- Smoking appears to lower breastmilk production by reducing prolactin levels. More women who smoke believe that they have insufficient milk than non-smokers.
- Mothers who smoke are likely to breastfeed for a shorter length of time.
- Many women continue to smoke whilst breastfeeding perceiving that it is the only time that they have for themselves, to overcome tiredness or to reduce their appetite.
- Passive smoking is related to early onset of wheezing although breastfeeding may reduce the severity of bronchial asthma. Research has shown that babies of mothers who smoke have three times more visits to GP with respiratory and sinus infection and allergy including asthma.
- Research shows exposure to smoke increases the risk of cot death in babies. If the mother and father smoke the risk is multiplied by seven.
- There have been reports linking smoking during breastfeeding with risk of obesity and endocrine dysfunction in the baby in later life.
So, there is no doubt that continuing to smoke whilst breastfeeding is harmful to your baby even if you or your partner don’t smoke in the same room as the baby, maybe even outside. Having said that breastfeeding and smoking still has benefits over not breastfeeding at all.
Behavioural Support
Behavioural support involves regular meetings with a trained person, usually a smoking cessation advisor. You are more likely to quit and remain as a non-smoker with behavioural support rather than trying to quit alone. The therapy is normally offered weekly for 4 weeks. It has also been called motivational interviewing – to help you stay motivated to quit. Normally the level of carbon monoxide (CO) in exhaled breath will be measured to show that you are quitting and as a positive feedback for you as you see the levels fall.
As an advisor I found on several occasions that I had a positive CO level at the end of the session, despite never having smoked, due to inhalation of second-hand smoke of the clients I was supporting many of whom had “one last cigarette” before the appointment!
How to change the habit of picking up a cigarette
We know that nicotine is highly addictive. However, with NRT there may still be a craving to pick up a cigarette at the times that you have normally smoked. These times may be a routine e.g., after a cup of coffee, after a meal. Think about where you smoke – is it always in the same place e.g., a chair you sit in, outside the kitchen door so in sight or sound of your baby but not with him/her.

It can help to identify when these times are for you and where you tend to smoke. I recommend keeping a diary for a week during which time you can also think about why you have decided to quit – is it for your baby, for your own health, because of the cost? Is it because you think you OUGHT to or have been told you SHOULD do so. If this has happened how do you feel about that? Shoulds and oughts are often hard to maintain. Plan to stop smoking rather than making a rapid decision on the spur of the moment, even with the best of intentions.
Decide how you can change each time you smoke – can you distract yourself for 20 minutes? This is the time it usually takes a craving to subside. Could you wash the floor, sing a song to your baby, make everything ready for the next meal, paint your nails or something else that works for you? If you smoke to give yourself “5 minutes peace” think about how else you could spend that time positively for you even if it is only to wee by yourself!
On the day you decide to stop, you may choose to tell everyone so that you gain their support, or you may want to keep quiet, so no-one tries to tempt you because they haven’t made their own decision. Some people just want to prove how hard it is and set you up to fail. Only you know whether your friends and family will help you or not.
I would also suggest putting the money that you would have spent on cigarettes in a savings box and at the end of 4 weeks or whatever period you decide, treat yourself to something you would have otherwise not been able to afford. Of course, you might choose that to be a family treat but remember it is also rewarding you for beating the addiction and craving. It isnt easy to give up smoking so be proud of yourself.
IF you have a cigarette one day at a point of weakness, be kind to yourself, accept the slip but carry on your intention to stop – one cigarette doesn’t mean you have failed, it is just one cigarette. Don’t stop giving up!
Have strong tasting sweets around to suck – traditionally these are mints but could be anything you like. Also have lots of healthy snacks so you don’t resort to chocolate or high calorie foods instead.
Nicotine Replacement Therapy (NRT) and Breastfeeding

- It is safer to use nicotine replacement therapy whilst breastfeeding than to smoke.
- Babies will be exposed to less nicotine through NRT than through smoking. Smoking produces blood levels of nicotine of 44ng/ml whilst NRT patches produce around 17 ng/ml.
- NRT avoids exposure to the other chemical compounds in tobacco smoke.
- Patches applied over a 24-hour period may produce vivid dreams in the mother; it might be advisable to remove the patch overnight so that the baby is exposed to less during night time feeds.
- NRT products do not cause breastmilk to smell of cigarettes.
- Nicotine gum produces large variations in nicotine levels whilst patches produce a sustained but lower level. If gum is used it should be chewed immediately after feeds to reduce the baby’s exposure. NRT nasal sprays similarly produce rapid high levels and may best be used after feeds.
- Exposure of the baby to NRT products is safer than exposure to cigarettes and with appropriate support may help the mother (and ideally her partner) to quit smoking permanently.
Medications to stop smoking and breastfeeding.
These tablets are not generally advised during breastfeeding but everyone has individual needs and they might be what is right for you.
Champix™ ( Varenicline)
• Varenicline is a partial nicotine agonist used to assist smoking cessation.
• One researcher points out that based on animal data on nicotine, varenicline might interfere with normal infant lung development and recommends against its use in nursing mothers.
• Based on its long half-life, poor protein binding and small molecular weight it is anticipated to transfer to human milk.
• Because no information is available on the use of varenicline during breastfeeding, an alternate drug is preferred, especially while nursing a new-born or preterm infant.
• If used monitor the baby for changes in sleep, changes in feeding, vomiting, constipation.
• For more information https://www.ncbi.nlm.nih.gov/books/NBK501688/
Zyban ™ (Bupropion)
• Limited information indicates that maternal bupropion doses of up to 300 mg daily produce low levels in breastmilk and would not be expected to cause any adverse effects in breastfed infants.
• However, there is little reported use in breastfed new-born infants and case reports of a possible seizure in partially breastfed 6-month-olds.
• If bupropion is required by a nursing mother, it is not a reason to discontinue breastfeeding.
• However, another drug may be preferred, especially while nursing a new-born or preterm infant.
• For more information https://www.ncbi.nlm.nih.gov/books/NBK501184/
Vaping and breastfeeding

A Cochrane review has found the strongest evidence yet that e-cigarettes, also known as ‘vapes’, help people to quit smoking better than traditional nicotine replacement therapies, such as patches and chewing gums.
E-cigarettes have become very popular as a safer alternative to cigarette smoking without exposure to tobacco and substances known to cause detrimental effects including lung cancer.
It was reported that an e-cigarette produced peak blood nicotine levels of 1.3 ng/mL in 19.6 minutes, which is comparable to the levels obtained by a nicotine inhaler (2.1 ng/mL in 32 minutes) and much lower than those obtained by a conventional cigarette (13.4 ng/mL in 14.3 minutes). This study further revealed that the reduction in the desire to smoke is similar to that of a nicotine inhaler but that e cigarettes are better tolerated by users.
The amount of nicotine delivered after 10 puffs of a 16 mg e cigarette is little to none. Based on these findings, it can be concluded that the amount of nicotine that transfers into breast milk after an acute inhalation of an e-cigarette is probably minimal, and comparable to that of a nicotine inhaler. But it is reported that an average e-cigarette user inhales up to 120 puffs/day.
Celebrate
Be proud of yourself – stopping smoking is not easy! Take every day as it comes and celebrate.

References
- Bullen C, McRobbie H, Thornley S, Glover M, Lin R, Laugesen M. Effect of an electronic nicotine delivery device (e cigarette) on desire to smoke and withdrawal, user preferences and nicotine delivery: randomised cross-over trial. Tob Control. 2010 Apr;19(2):98-103.
- Eissenberg T. Electronic nicotine delivery devices: ineffective nicotine delivery and craving suppression after acute administration. Tob Control. 2010 Feb;19(1):87-88)
- Etter JF, Bullen C. Electronic cigarette: users’ profile, utilization,satisfaction and perceived efficacy. Addiction. 2011 Nov;106(11):2017-2028
- Gov.UK Smokers urged to swap cigarettes for vapes in world first scheme https://www.gov.uk/government/news/smokers-urged-to-swap-cigarettes-for-vapes-in-world-first-scheme
- NHS Digital Statistics on Women’s Smoking Status at Time of Delivery: England Quarter 4, 2020-21
- NHS Stop smoking in pregnancy https://www.nhs.uk/pregnancy/keeping-well/stop-smoking
- NIHR Smoking and Addiction https://evidence.nihr.ac.uk/alert/e-cigarettes-better-than-nicotine-patches-helping-pregnant-women-stop-smoking/
- Tappin D, Sinclair L, Kee F, McFadden M, Robinson-Smith L, Mitchell A et al. Effect of financial voucher incentives provided with UK stop smoking services on the cessation of smoking in pregnant women (CPIT III): pragmatic, multicentre, single blinded, phase 3, randomised controlled trial BMJ 2022; 379 :e071522 doi:10.1136/bmj-2022-071522
- Zhao L et al. Parental smoking and the risk of congenital heart defects in offspring: An updated meta-analysis of observational studies. 2020; RCP. Hiding in plain sight: treating tobacco dependency in the NHS. 2018; Pineless BL et al. Systematic review and meta-analysis of miscarriage and maternal exposure to tobacco smoke during pregnancy. 2014; RCP & RCPCH. Passive Smoking and Children. 2010
Migraine and breastfeeding powerpoint
I delivered this presentation for Migraine Ireland and will upload it onto YouTube but sharing the powerpoint slides for training purposes. Happy to answer any questions wendy@breastfeeding-and-medication.co.uk
Available on YouTube https://youtu.be/Lg52tht4XwU

Zuranolone (Zurzuvae™) and Breastfeeding
Back in August 2023 I posted about a new drug Zuranolone licensed by the FDA in USA to treat perinatal depression. The course lasts just 2 weeks but the manufacturer was recommending that mothers shouldn’t breastfeed on it or for a week after.
However, this afternoon (September 2023)I was listening to a webinar by Dr Tom Hale and Dr Kaytlin Krutsch where they presented data on 15 women who took it but pumped throughout.
“The manufacturer reports minimal transfer into breast milk. The concentration of drug-in-milk quantified in the milk was not disclosed; however, the mean RID was reported as 0.357% at day 5 (dose unknown; 30 to 50 mg per day). The oral bioavailability of zuranolone is unknown, but the reported RID% would likely result in negligible infant exposure.
Zuranolone has a dose-dependent abuse potential; patients report feeling euphoric mood, feeling drunk, and somnolence with zuranolone use. Adverse effects upon discontinuing the drug in the mother may include mild-to-moderate insomnia, palpitations, decreased appetite, paranoia, hyperhidrosis, nausea, and more. For the mother, there is a risk of excessive sedation with the potential inability of the mother to assess the degree of their impairment. This was not noticed in the lactation study. Instead, patients reported mild dizziness and potential memory loss during the treatment.[Poster: An open-label study to evaluate concentrations of zuranolone in the breastmilk of healthy lactating women. Available upon request to the manufacturer. Sage Therapeutics/BioGen Inc. 2021.]
Progesterone is thought to inhibit lactation. Researchers reported the average milk volume trended 8.3% down from a mean of 526 mL on day 1 to 485 mL on day 3 to 5 (when steady-state was reached). Moms were required to exclusively pump for the trial, which may partially explain the drop in volume.”
It is recommended that the baby so exposed through milk is monitored for sedation.
see also LactMed https://www.ncbi.nlm.nih.gov/books/NBK594292/
“Because of the low amounts of zuranolone in milk, it would not be expected to cause any adverse effects in breastfed infants. If zuranolone is required by the mother, it is not a reason to discontinue breastfeeding. Until more data are available, zuranolone should be used with careful infant monitoring for excessive sedation during breastfeeding, especially with higher dosages and in newborn and preterm infants.”
“The manufacturer reports a study in 14 healthy lactating women treated with oral administration of 30 mg of zuranolone daily for 5 days. The daily infant dose was approximately 0.0013 mg/kg, resulting in a mean weight-adjusted relative infant dose of 0.357% compared to the maternal dose. Concentrations of zuranolone in breastmilk were below the level of quantification limit by 4 to 6 days after the last dose.”
To my knowledge this drug is not yet approved in the UK.
- Mahase E US approves daily pill for postpartum depression https://www.bmj.com/content/382/bmj.p1822
- Perinatal depression: a neglected aspect of maternal health https://www.thelancet.com/pdfs/journals/lancet/PIIS0140-6736(23)01786-5.pdf
- Deligiannidis KM, Meltzer-Brody S, Gunduz-Bruce H, et al. Effect of Zuranolone vs Placebo in Postpartum Depression: A Randomized Clinical Trial. JAMA Psychiatry. 2021;78(9):951–959.
- Deligiannidis KM, Meltzer-Brody S, Gunduz-Bruce H, Doherty J, Jonas J, Li S, Sankoh AJ, Silber C, Campbell AD, Werneburg B, Kanes SJ, Lasser R. Effect of Zuranolone vs Placebo in Postpartum Depression: A Randomized Clinical Trial. JAMA Psychiatry. 2021 Sep 1;78(9):951-959. doi: 10.1001/jamapsychiatry.2021.1559. Erratum in: JAMA Psychiatry. 2022 Jul 1;79(7):740. Erratum in: JAMA Psychiatry. 2023 Feb 1;80(2):191. PMID: 34190962; PMCID: PMC8246337.
- An open-label study to evaluate concentrations of zuranolone in the breastmilk of healthy lactating women. Available upon request to the manufacturer. Sage Therapeutics/BioGen Inc. 2021
Phenylephrine and Breastfeeding
I have written extensively about the use of decongestants in the past ( https://breastfeeding-and-medication.co.uk/fact-sheet/coughs-colds-flu-and-covid-when-breastfeeding and https://www.breastfeedingnetwork.org.uk/factsheet/decongestants/)
Pseudoephedrine has been shown to reduce milk supply in some women. The effect of phenylephrine on supply has not been demonstrated but use of oral decongestants is generally not advised for breastfeeding women.
I have always recommended the use of nasal sprays as decongestants together with the use of steam inhalation as being more effective than oral medication and with no potential impact on supply.
In September 2023 the FDA reported that oral phenylephrine is not effective at relieving nasal stuffiness. It is important to note that neither FDA nor the Non-prescription Drug Advisory Committee raised concerns about safety issues with use of oral phenylephrine at the recommended dose. (https://www.fda.gov/drugs/drug-safety-and-availability/fda-clarifies-results-recent-advisory-committee-meeting-oral-phenylephrine).
According to one USA website the evidence for efficacy was first questioned in 2007. The manufacturers have cited a survey that many people find its use beneficial as shown by sales volume of cough and cold products.
The vote that formally declared phenylephrine ineffective was in line with a review of pharmacology and clinical data presented by the FDA, which found the oral bioavailability of the drug is less than 1%, compared with 38%, a number often cited in the literature and based on outdated technology. (Medscape https://www.medscape.com/viewarticle/996369).
There appears to be no current UK recommendations although I am sure there is current discussion. Most oral cough and cold remedies currently contain phenylephrine as pseudoephedrine sales have been restricted. Between 2007 and 2008, the government introduced restrictions on their use because of concern that medicines containing these active substances could be used in the illicit manufacture of the Class A controlled drug methylamphetamine https://www.gov.uk/drug-safety-update/pseudoephedrine-and-ephedrine-update-on-managing-risk-of-misuse#:~:text=Sales%20restrictions,-Since%20April%202008&text=It%20is%20illegal%20to%20sell,mg%20ephedrine%20without%20a%20prescription
This information has been compiled from a variety of sources and does not imply recommendation other than that nasal decongestants and steam inhalation are effective in reducing symptoms of nasal congestion during breastfeeding without potential impact on supply. Most of us have our own preferred remedies which we find effective and that remains a personal choice





